Origins of Personality Disorders
The cause of personality disorders is unknown. However, we do know that personality disorders are highly related to early child hood trauma, which can take the form of emotional, physical or sexual abuse, inconsistent parenting, and/or parental neglect (Dudeck, et. al., 2007; Griffin, 2004; Grover, et. al. 2007; Johnson, Sheahan, & Chard, 2003; Mclean & Gallop, 2003; Minzenberg, Poole, & Vinogradov, 2006; Modestin, 2006; Narisco, 2007; Seese, 1997; Semiz, Basoglu, Ebrinc, & Cetin, 2007) [1]. A study of personality disordered outpatients (who tend to have less severe symptoms) by Bierer, et. al. (2003) found only modest relationships between specific trauma dimensions and personality disorder diagnoses, though the general relationship between trauma and personality disorders was high. Sexual and physical abuse were specific predictors of paranoid and antisocial personality disorders, while emotional abuse predicted borderline personality disorder.
Interestingly enough, childhood sexual abuse does not seem to cause neuro-biological changes in people suffering from borderline personality disorder (Zweig-Frank, et. al., 2006), though numerous studies have now demonstrated neurological differences in personality disordered patients compared to normal controls (see section below).
Genetic and other environmental factors play important roles in the characteristics of some personality disorders. For instance, borderline personality disorder itself does not seem to be genetically determined and research has shown that most people with borderline personality disorder have suffered from abuse as children and that memories of this abuse are stable (Kremers, et. al. 2007). Nevertheless, some the key characteristics of this disorder, such as aggressiveness, impulsivity, suicidal tendencies, and emotional instability have been shown to be heritable (Coccaro, Bergman & McLean 1993; Bohman, et. al., 1984; Bouchard, 1994; Machizawa-Summers, 2007; Silverman, et. al., 1991; Togersen, et al, 1994; Torgersen, 2000).
A rule of thumb is ‘the worse the childhood the worse the personality disorder’, (Modestin, 2006; Vizard, Hickey, & McCrory, 2007) with more severe personality disorders being co-morbid with dissociative disorders (Sar, et. al., 2006). In another study childhood trauma and dissociative experience among patients with borderline personality disorder was related to emotional and physical abuse, and emotional neglect. Patients labeled as ‘high dissociators’ reported significantly greater levels of emotional/physical abuse, and emotional/physical neglect than low dissociators. Sexual abuse was not significantly related to dissociative experiences (Watson, et. al. 2006). In fact one study has demonstrated that people diagnosed with borderline personality disorder who do not report childhood sexual abuse are likely to achieve remission of the disorder in a relatively short amount of time Zanarini, et. al., 2006) [2].
At the more severe end of the personality disorder spectrum the patient may experience transient psychotic states. For patients at the severe end of this spectrum the distinction between a personality disorder and a psychosis can become a bit academic (Newton-Howes, et. al. 2008).
Neurobiology of Personality Disorders
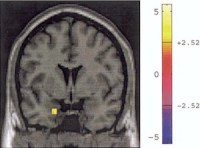
There is quite a bit of promising research on personality disorders that examines the development of the brain. Traumatic events and/or inconsistent parenting are theorized to cause changes in the nerve pathways from the part of the brain where emotions are generated through the cerebral cortex where the emotions are regulated. As people with personality disorders have difficulty regulating emotions it is thought that areas of the brain related to emotional regulation may be dysfunctional. Using state of the art imaging technologies such as fMRI (functional magnetic resonance imaging) researchers have been able to show difference in brain function between people diagnosed with personality disorders and normal volunteers. This research not only gives hope for the development of new kinds of medication that may help personality disordered people better regulate their emotional states, but also may clarify the role of emotional regulation in human beings.
 One interesting line of research theorizes that neurological mechanisms underlying personality disorders may have evolved to help a person (really a child) adapt to a chaotic external environment. Lack of various types of empathy may have had survival value at different times in human evolution (Smith, 2006). In a chaotic, unstable, environment – say for instance a war zone – being in ‘fight or flight’ mode, labile emotional states and the ability to dissociate from one’s emotions, may have survival value (Austin, Riniolo, & Porges, 2007, Troisi, 2007). These kinds of chaotic and uncertain environments have characterized much of human and primate history. The deep and inherent nature of these mechanisms would also help explain why personality disorders are so very difficult to work with.
One interesting line of research theorizes that neurological mechanisms underlying personality disorders may have evolved to help a person (really a child) adapt to a chaotic external environment. Lack of various types of empathy may have had survival value at different times in human evolution (Smith, 2006). In a chaotic, unstable, environment – say for instance a war zone – being in ‘fight or flight’ mode, labile emotional states and the ability to dissociate from one’s emotions, may have survival value (Austin, Riniolo, & Porges, 2007, Troisi, 2007). These kinds of chaotic and uncertain environments have characterized much of human and primate history. The deep and inherent nature of these mechanisms would also help explain why personality disorders are so very difficult to work with.
The idea that personality disorders have at least a partially neurological genesis is not new. As early as 1946, Estabrooks theorized that strong emotional shocks, especially in childhood could ‘sensitize’ the brain causing personality disorders:
It matters little if the photographic plate of the brain, to use a very crude analogy, is exposed once in blinding light or 100 times in to the same object in dim light. The impression is, in the long run, just as definite and just as permanent (Estabrook, 1946, p. 204).
Modern views of personality disorders hypothesize that genetics, childhood trauma (and other environmental factors) are related to the characteristics of personality disorders such as emotional instability, impulsivity, aggression, and possibly cognitive and perceptual problems. These views have been arrived at not only through psychological studies, but increasingly through research on brain chemistry and structure (Goyer, Konicki, & Schultz, 1994).
One of the personality disorders most often studied is borderline personality disorder. Besides the obvious importance for understanding this destructive disorder the characteristics of the disorder lend themselves to better operational definition than the characteristics of other personality disorders. Typically, researchers have looked at impulsivity, aggression, (as well impulsive aggression), emotional instability, self-mutilation, and suicidal behaviors as indicators of borderline personality disorder. It may be that reduced serotonin transmission capacity in the brain may contributes to these negative traits among people suffering from borderline personality disorder. There is also research that suggests that the cholinergic system may be related to emotional instability, but that more work needs to be done to understand the physiology of this phenomenon. (Leyton, et. al. 2001; New & Siever, 2002; Zaboli, et. al., 2006).
A recent review of the research in this area conclude that impulsive aggression may involve deficits in central serotonin function as well as changes in the cingulate and medial and orbital prefrontal cortex. While these changes are hypothesized to be caused by early childhood trauma, this has not yet been definitively demonstrated. Borderline personality disorder has been shown to be biologically distinct from post-traumatic stress so the role of specific trauma is not yet known. Nevertheless, people with borderline personality disorder typically suffer from high rates of childhood abuse and neglect. It may be that the contribution of specific instances of trauma are less important than an overall long-term pattern of abuse in childhood. Studies of gene alterations that cause a reduction in serotonin have been shown to moderately affect impulsive and aggressive behavior and indicate that these aspects of borderline personality disorder may be inherited traits (Goodman, New & Seiver, 2004).
It may be true that people with the serotonin reducing genes may be more highly susceptible to traumatic childhood environment. A study by Reif, et. al. (2007) also found that genetic polymorphisms related to reduced serotonergic neurotransmission were related to violent behavior. The authors found that 45% of subjects carrying the low serotonin activity allele were prone to violent behavior compared to 30% with the normal serotonin activity allele. Subjects with the low serotonin activity allele who had experienced a highly adverse childhood environment were more likely to be violent later in life.
Brendel, Stern, & Silbersweig (2005) examined the interaction between negative emotion and lack of behavioral control. The authors report that abnormal frontolimbic circuitry is a likely suspect that explains the major clinical features of borderline personality disorder. These neuroimaging findings are integrated with developmental perspectives to explain the pathology associated with borderline personality syndrome, including the ways in which early childhood experience may interact with the developing brain.
The research on structural aspects of the brain also has demonstrated key differences in the brain of borderline personality sufferers when compared to normal people. One recent study by Silbersweig, et. al. (2007) examined impulse control in people with borderline personality disorder using functional magnetic resonance imaging technology. In order to assess impulse control the researchers asked subjects not to push a button when negative words were displayed. Normal subjects showed increased activity in the areas of the brain associated with emotional regulation and inhibition of limbic regions including the amygdala (orbitofrontal and cigulate cortices). These increases did not occur in people who suffered from borderline personality disorder. Also those with borderline personality disorder demonstrated increased activity in areas of the brain (dorsal anterior cingulated cortex) related to detection of conflict related to deciding on a response, suggesting that while they were unable to exercise impulse control, they had some awareness of the conflict inherent in the experimental situation. The research leads us to
…infer that when individuals with borderline personality disorder display decreased impulse control, this loss of impulse control may reflect a deficit in recruitment of brain mechanism of emotional regulation, and this process may be potentiated by context. Particularly stressful or negative contexts could lead to more impaired impulse control (Siegle, 2007, p. 1778).
Interestingly, the brain regions related to borderline personality disorder are also implicated in depression. Not surprisingly, borderline personality disorder and depression are often co-morbid. This suggests that treatment that works for some affective disorders may also help in borderline personality disorder. This may especially be true if contextual factors related to impulse control are included in the therapeutic regime (Brendel, Stern, & Silbersweig, 2005), and may explain why treatment such as Dialectic Behavior Therapy has proven successful with people suffering from borderline personality disorder (Siegle, 2007).
Next – Culture & Conclusions
References
Austin, M. A., Riniolo, T. C., & Porges, S. W. (2007). Borderline personality disorder and emotion regulation: Insights from the Polyvagal Theory. Brain and Cognition, 65(1), 69-76. doi: 10.1016/j.bandc.2006.05.007.
Bierer, L. M., Yehuda, R., Schmeidler, J., Mitropoulou, V., New, A. S., Silverman, J. M., & Siever, L. J. (2003). Abuse and Neglect in Childhood: Relationship to Personality Disorder Diagnoses. CNS Spectrums, 8(10), pp. 737-740.
Bohman, M., Cloniger, C.R., von Knorring, A., & Sigvardsson, S. (1984). An adoption study of somatoform disorders III: Cross-fostering analysis and genetic relationship to alcoholism and criminality. Archives of General Psychiatry, 41, pp. 872-878.
Bouchard, T.J. (1994). Genes, environment and personality. Science, 264(5166), 1700-1701.
Brendel, G. R., Stern, E., & Silbersweig, D. A. (2005). Defining the neurocircuitry of borderline personality disorder: Functional neuroimaging approaches. Development and Psychopathology, 17(4), pp. 1197-1206.
Coccaro, E.F., Bergman, C.S., & McLean, G.E. (1993). Heritability of irritable impulsiveness: A study of twins reared together and apart. Psychiatry Research, 48(3), p. 229-242.
Dudeck, M., Spitzer, C., Stopsack, M., Freyberger, H.J., & Barnow, S. (2007). Forensic inpatient male sexual offenders: The impact of personality disorder and childhood sexual abuse. Journal of Forensic Psychiatry & Psychology, 18(4), pp. 494-506.
Estabrooks, G.H. (1946). Brain sensitization in personality disorders. The Journal of General Psychology, 34, pp. 203-211.
Goodman, M., New, A., & Siever, L. (2004). Trauma, Genes, and the Neurobiology of Personality Disorders. In Yehuda, R., & McEwen, B. Biobehavioral stress response: Protective and damaging effects. New York, NY: New York Academy of Sciences, pp. 104-116.
Goyer, P. F., Konicki, P. E., & Schulz, S. C. (1994). Brain imaging in personality disorders In Silk, K. R. Biological and neurobehavioral studies of borderline personality disorder. Washington, DC: American Psychiatric Association, pp. 109-125.
Griffin, J. L. (2004). Structural equation modeling of Borderline Personality Disorder: Cognitive distortions, maladaptive schemas, psychological distress and insecure attachment as long-term sequelae of childhood sexual abuse. Dissertation Abstracts International: Section B: The Sciences and Engineering, 64(10-B), pp. 5216.
Grover, K.E., Carpenter, L.L., Price, L.H., Gagne, G.G., Mello, A.F., Mello, M.F., & Tyrka, A.R. (2007). The relationship between childhood abuse and adult personality disorder symptoms. Journal of Personality Disorders, 21(4), pp. 442-447.
Johnson, D. M., Sheahan, T. C., & Chard, K. M. (2003). Personality Disorders, Coping Strategies, and Posttraumatic Stress Disorder in Women with Histories of Childhood Sexual Abuse. Journal of Child Sexual Abuse, 12(2), pp. 19-39.
Kremers, I. P., Van Giezen, A. E., Van der Does, A. J. W., Van Dyck, R., & Spinhoven, P.H. (2007). Memory of childhood trauma before and after long-term psychological treatment of borderline personality disorder. Journal of Behavior Therapy and Experimental Psychiatry, 38(1), pp. 1-10.
Leyton, M. L., Okazawa, H. O., Diksic, M., Paris, J., Rosa, P., Mzengeza, S., Young, S. N., Blier, P., & Benkelfat, C. (2001). Brain regional [11C] methyl-L-tryptophan trapping in impulsive subjects with borderline personality disorder. American Journal of Pyshciatry, 158(5), 775-782.
Machizawa-Summers, S. (2007). Childhood trauma and parental bonding among Japanese female patients with borderline personality disorder. International Journal of Psychology, 42(4), Aug 2007. pp. 265-273.
McLean, L. M., Gallop, R. (2003). Implications of childhood sexual abuse for adult borderline personality disorder and complex posttraumatic stress disorder. American Journal of Psychiatry, 160(2), pp. 369-371.
Millon, T., Blaneyu. P. H., & Davis R. (eds.) (1999). Oxford Textbook of Psychopathology. New York: Oxford University Press. pp. 510.
Minzenberg, M. J. Poole, J. H., & Vinogradov, S. (2006). Adult social attachment disturbance is related to childhood maltreatment and current symptoms in borderline personality disorder. Journal of Nervous and Mental Disease, 194(5), pp. 341-348.
Modestin, J. (2006). Aetiology of personality disorders. Schweizer Archiv für Neurologie und Psychiatrie, 157(5), Jun 2006. pp. 221-226.
Narcisco, B. (2007). The relationships among trauma, self-concept, dissociation, Cluster B Personality Disorders and adult attachment style in incarcerated women. Dissertation Abstracts International: Section B: The Sciences and Engineering, 68(1-B), pp. 630.
Newton-Howes G, Tyrer P, North B, Yang M. (2008). The prevalence of personality disorder in schizophrenia and psychotic disorders: systematic review of rates and explanatory modelling. Preview Psychological Medicine, 38(8), pp. 1075-1082.
Reif, A., Rosler, M., Freitag, C. M., Schneider, M., Eujen, A. Kissing, C., Wenzler, D., Jacob, C. P., Retzt-Junginger, P., Thome. J., Lesch, K. P., & Retz. W. (2007). Nature and Nurture Predispose to Violent Behavior- Serotonergic Genes and Adverse Childhood Environment. Neuropsychopharmacology, 32, pp. 2375–2383.
Sar, V., Akyuz, G., Kugu, N., Ozturk, E., Ertem-Vehid, H. (2006). Axis I dissociative disorder comorbidity in borderline personality disorder and reports of childhood trauma. Journal of Clinical Psychiatry, 67(10), pp. 1583-1590.
Semiz, U., Basoglu, C., Cetin, M., Ebrinc, S., Uzun, O., & Ergun, B. (2008). Body dysmorphic disorder in patients with borderline personality disorder: prevalence, clinical characteristics, and role of childhood trauma. Acta Neuropsychiatrica, 20(1), pp. 33-40.
Siegle, G. J. (2007). Brain mechanisms of borderline personality disorder at the intersection of cognition, emotion, and the clinic. American Journal of Psychiatry, 164(12), pp. 1776-1779.
Silbersweig, D., Clarkin, J. F., Goldstein, M., Kernberg, O. F.,Tuescher, O., Levy, K. N., Brendel, G., Pan, H., Beutel, M., Pavony, M. T., Epstein, J., Lenzenweger, M. F., Thomas, K. M., Posner, M. I., & Stern, E. (2007). Failure of frontolimbic inhibitory function in the context of negative emotion in borderline personality disorder. American Journal of Psychiatry, 164(12), pp. 1832-1841.
Silverman, J.M., Pinkham, L., Horvath, T.B., Coccaro, E.F., Howard, K., Schear, S., Apter, S., Davidson, M., Mohs, R., & Siever, L.J. (1991). Affective and impulsive personality disorder traits in the relatives of patients with borderline personality disorder. American Journal of Psychiatry, 148(10), p. 1378-1385.
Smith, A. (2006). Cognitive empathy and emotional empathy in human behavior and evolution. Psychological Record, 56(1), 3-21.
Torgersen, S. (2000). Genetics of patients with borderline personality disorder. Psychiatric Clinics of North America, 23(1), p. 1-9.
Torgersen, S. (1984). Genetic and nosological aspects of schizotypal and borderline personality disorders: A twin study. Archives of General Psychiatry, 41(6), p. 546-554.
Troisi, A. (2007). The relevance of personality disorders for an evolutionary genetics of personality. European Journal of Personality, European personality reviews 2007., 21(5), 633-635.
Vizard, E., Hickey, N., & McCrory, E. (2007). Developmental trajectories associated with juvenile sexually abusive behaviour and emerging severe personality disorder in childhood: 3-year study. British Journal of Psychiatry: Special issue: Assessment, risk and outcome in severe personality disorder, 190(Suppl 49), pp. s27-s32.
Watson, S., Chilton, R., Fairchild, H., & Whewell, P. (2006). Association between childhood trauma and dissociation among patients with borderline personality disorder. Australian and New Zealand Journal of Psychiatry, 40(5), pp. 478-481.
Zaboli, G., Gizatullin, R., Nilsonne, A., Wilczek, A., Jonsson, E. G., Ahnemark, E., Asberg, M, & Leopardi, R., (2006). Tryptophan hydroxylase-1 gene variants associate with a group of suicidal borderline women. Neuropsychopharmacology, 31, pp. 1982-1990.
Zanarini, M. C. Frankenburg, F. R. Hennen, J., Reich, D. B., & Silk, K. R. (2006). Prediction of the 10-Year Course of Borderline Personality Disorder. American Journal of Psychiatry, 163(5), pp. 827-832.
Zweig-Frank, H., Paris, J., Kin, N. Y., Schwartz, G., Steiger, H., & Nair, N. V. (2006). Childhood sexual abuse in relation to neurobiological challenge tests in patients with borderline personality disorder and normal controls. Psychiatry Research, 141(3), 337-341. doi:10.1016/j.psychres.2005.02.009
—————
1. Literally hundreds of studies could have been listed here to support this statement. I have chosen to list only a few recent examples.
2. This also calls into question the reliability of the methods used for determining a diagnosis of borderline personality syndrome and would suggest that the predictors found in this study be used to rule out diagnosis of this disorder
—————